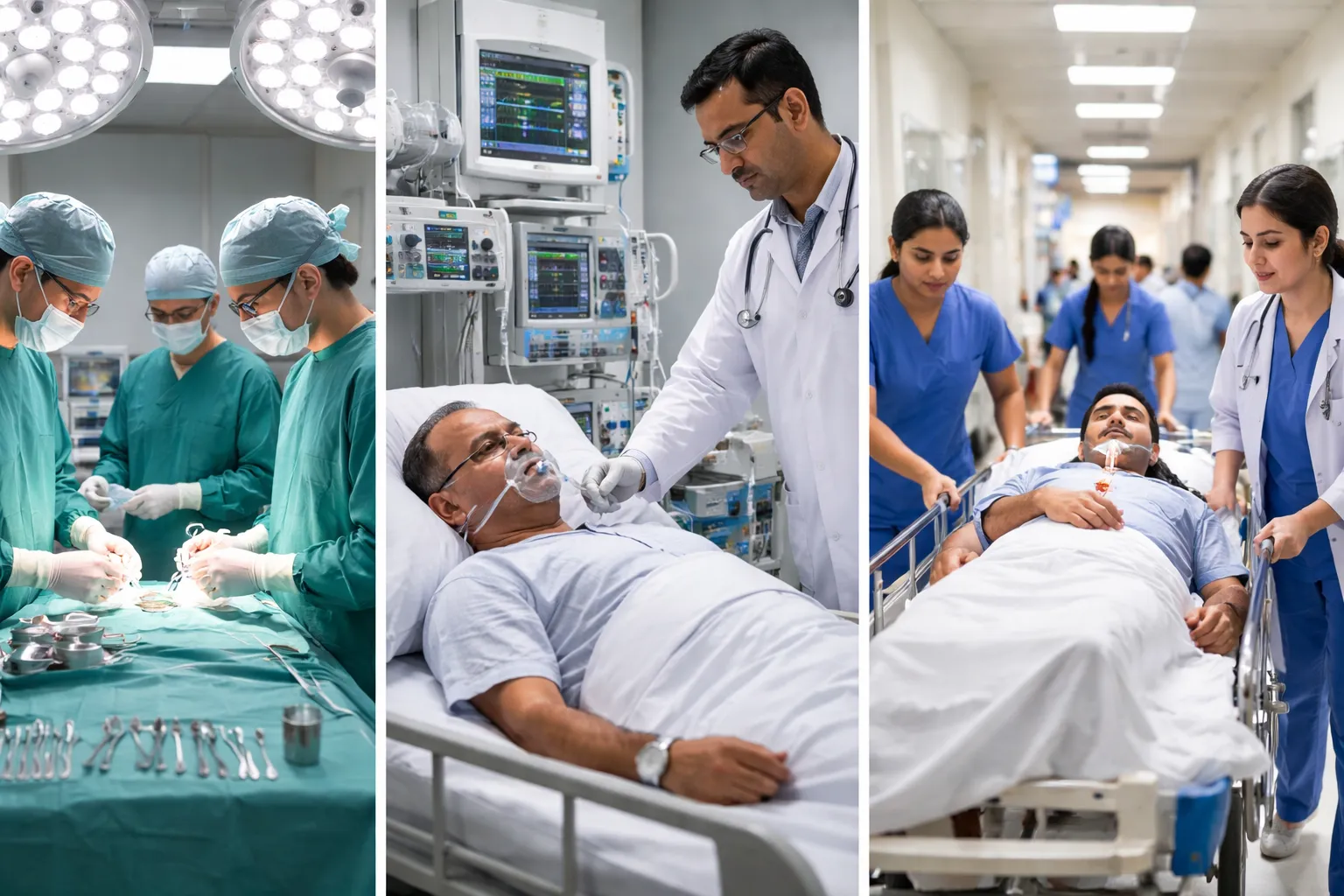
NABH Standards for OT, ICU & Emergency Departments: A Complete Guide
If you work in a hospital or are running one, you already know that quality care is not optional. It is the foundation of every patient interaction. In India, the National Accreditation Board for Hospitals & Healthcare Providers (NABH) is the gold standard when it comes to hospital quality and patient safety. Getting your OT, ICU, or Emergency Department up to NABH standards is one of the most important steps any healthcare institution can take. But what does that actually mean in practice?
This article breaks it all down for you, in plain language. Whether you are a hospital administrator, a clinician, a quality manager, or just someone curious about how Indian hospitals maintain safety standards, this guide covers what NABH expects from your Operation Theatre, Intensive Care Unit, and Emergency Department.
What Is NABH and Why Does It Matter?
NABH is a constituent board of the Quality Council of India (QCI). It was set up to establish and operate accreditation programs for healthcare organizations. You can explore the full scope of accreditation programs directly on the NABH official website. Hospitals that earn NABH accreditation meet specific, measurable standards across all departments. These standards cover everything from patient rights to infection control, staff qualifications to medical record keeping.
NABH accreditation signals to patients and health insurance providers that your hospital has been evaluated by an independent body and found to meet high-quality benchmarks. For hospitals, it also leads to better processes, fewer medical errors, and improved patient outcomes. If you are still in the early stages of understanding what the accreditation process looks like from start to finish, this step-by-step NABH accreditation guide for new hospitals is a great place to start. In short, it is a win for everyone involved.
NABH Standards for the Operation Theatre (OT)
The Operation Theatre is where surgical procedures happen, and with that comes a significant level of risk. NABH has laid out detailed standards to make sure that each surgery is conducted safely, with the right checks, the right environment, and the right people in place.
Pre-Operative Assessment Requirements
Before a patient even enters the OT, NABH expects hospitals to complete a thorough pre-operative assessment. This includes:
- Medical history review and physical examination by the operating surgeon
- Anesthesia pre-assessment by a qualified anesthesiologist
- Relevant investigations like blood tests, ECG, and imaging reports
- Informed consent documentation signed by the patient or legal guardian
- Assessment of comorbid conditions that may affect surgical outcomes
The pre-operative checklist is not just a formality. It is a real safeguard that helps catch problems before they become critical inside the operation theatre.
Surgical Safety Checklist
NABH strongly aligns with the WHO Surgical Safety Checklist, which is divided into three phases: Sign In (before anesthesia), Time Out (before incision), and Sign Out (before the patient leaves the OT). Each phase has specific verification steps.
| Phase | Key Checks |
|---|---|
| Sign In | Patient identity, site marking, consent, anesthesia machine check, allergy review |
| Time Out | Team introduction, procedure confirmation, antibiotic prophylaxis, critical steps discussion |
| Sign Out | Instrument count, specimen labeling, equipment issues noted, post-op care plan discussed |
OT Environment and Infrastructure Standards
NABH lays out clear expectations for how the OT must be physically set up. Getting these structural elements right from the ground up is something that requires careful planning, which is why hospital planning and designing plays such a critical role before the first brick is even laid:
- Positive pressure ventilation with HEPA filtration in major OTs
- Separate zones: sterile, clean, and disposal areas
- Proper temperature and humidity controls
- Adequate lighting, including backup power for critical equipment
- Separate entry and exit pathways to prevent cross-contamination
Sterilization and Infection Control in the OT
Surgical site infections (SSIs) are one of the most common healthcare-associated infections. NABH sets strict guidelines around sterilization practices. All surgical instruments must go through validated sterilization methods (autoclave, ETO, or plasma sterilization, depending on the item). Sterility assurance level (SAL) must be maintained with proper documentation, biological indicators used for each cycle, and records kept for audit purposes.
Key OT Infection Control Practices Under NABH
- Scrub protocols for surgical team members
- Maintenance of sterile field throughout the procedure
- Antibiotic prophylaxis as per hospital policy and clinical guidelines
- Regular environmental cultures to detect contamination
- Defined policy for handling implants and single-use devices
Let’s Build Your Dream Hospital
Whether you’re planning a new hospital, expanding an existing facility, or upgrading your healthcare technology, Actiss Healthcare is here to guide you every step of the way. Let us help you turn your vision into reality. Contact us today for a free consultation & learn more about our services and how we can support your next healthcare project.

NABH Standards for the Intensive Care Unit (ICU)
The ICU is a high-stakes environment. Patients here are critically ill, often dependent on life-support equipment, and need round-the-clock monitoring. NABH has detailed standards that govern how an ICU must be set up and run.
ICU Admission and Discharge Criteria
One of the foundational NABH requirements is that every ICU must have written, approved criteria for admitting and discharging patients. This protects against inappropriate use of ICU resources and ensures that critically ill patients get timely access to beds. Admission criteria usually include:
- Hemodynamic instability requiring vasopressor support
- Respiratory failure requiring mechanical ventilation
- Post-operative monitoring after high-risk surgeries
- Multi-organ dysfunction syndrome
Discharge criteria include clinical stability, weaning from monitoring devices, and the availability of an appropriate step-down care area.
Staffing Ratios and Qualification Standards
NABH is particular about who runs your ICU. The standard requires that:
- A qualified intensivist or senior physician must be available 24/7 either in-house or on-call
- Nurse-to-patient ratios must be maintained (typically 1:1 or 1:2 for level III ICUs)
- At least one trained ICU nurse per shift
- ICU nurses must have formal critical care training or certification
Proper staffing is not just about meeting a number on paper. It directly impacts mortality rates and patient outcomes in the ICU, and NABH auditors check this closely.
Equipment and Monitoring Standards
Every ICU bed unit under NABH must have the right equipment in place and functional at all times. Selecting and procuring the correct medical technology for an ICU is a specialized task, and working with a healthcare technology consultancy can help hospitals avoid expensive procurement mistakes:
- Multi-parameter bedside monitor (ECG, SpO2, NIBP, temperature, IBP if needed)
- Infusion pumps and syringe pumps
- Ventilator (at least one per ICU, ideally per bed in Level III)
- Defibrillator with pacing function
- Emergency drug tray maintained and checked daily
Infection Prevention in the ICU
Healthcare-associated infections (HAIs) in the ICU are a serious problem worldwide. NABH standards require hospitals to actively track and reduce VAP (Ventilator-Associated Pneumonia), CAUTI (Catheter-Associated Urinary Tract Infection), and CLABSI (Central Line-Associated Bloodstream Infection).
| HAI Type | Prevention Bundle |
|---|---|
| VAP | Head elevation 30-45°, oral decontamination, sedation vacation, daily extubation assessment |
| CAUTI | Aseptic insertion, closed drainage system, daily review of catheter necessity |
| CLABSI | Hand hygiene, maximal barrier precautions, chlorhexidine skin prep, daily line review |
Documentation and Care Planning in ICU
NABH expects detailed documentation in ICU settings. This includes daily ICU notes, fluid balance charts, ventilator parameters, sedation and analgesia scores (like RASS and NRS), nutritional assessment, and multidisciplinary rounds notes. Family communication records are also expected as part of patient-centered care.
NABH Standards for the Emergency Department (ED)
The Emergency Department is often the first point of contact for seriously ill patients. Getting care right here can mean the difference between life and death. NABH standards for the ED are shaped around speed, accuracy, and safety.
Triage System Requirements
NABH mandates that every Emergency Department must have a formal triage system in place. Most NABH-accredited hospitals use either the Manchester Triage System (MTS) or a 5-level triage model. The purpose is to categorize patients by urgency so the most critical ones are seen first.
Common Triage Categories Used in NABH-Accredited EDs
- Category 1 (Immediate/Red): Life-threatening, seen within 0 minutes
- Category 2 (Emergent/Orange): Very urgent, seen within 10 minutes
- Category 3 (Urgent/Yellow): Urgent, seen within 30 minutes
- Category 4 (Semi-urgent/Green): Less urgent, seen within 60 minutes
- Category 5 (Non-urgent/Blue): Non-urgent, seen within 120 minutes
Resuscitation Area Standards
Every NABH-compliant Emergency Department must have a dedicated resuscitation bay or crash area. This zone must be stocked and ready at all times, with:
- Crash cart with defibrillator and all ACLS drugs
- Airway management equipment (bag-valve mask, laryngoscope, ET tubes, video laryngoscope if possible)
- Ventilator or transport ventilator
- Intravenous access supplies and fluid resuscitation options
- Point-of-care testing equipment for quick labs
The crash cart must be checked every shift. This is a non-negotiable requirement under NABH and auditors will ask for the crash cart check registers during assessments.
Trauma Care and Mass Casualty Protocols
NABH expects hospitals with Emergency Departments to have a documented Mass Casualty Incident (MCI) plan. This plan outlines how the hospital will handle a sudden influx of patients (from road accidents, industrial disasters, etc.). The plan must be rehearsed through regular mock drills, and records of those drills must be maintained.
ED Documentation and Handover Standards
Proper documentation in the Emergency Department is a core NABH requirement. This includes:
- Time-stamped triage records
- Initial assessment notes
- Consent for procedures performed in the ED
- Clear handover documentation when transferring patients to wards or ICU
- Record of patients who left against medical advice (LAMA) with appropriate counseling noted
Comparing Key NABH Requirements Across OT, ICU, and Emergency
| Area | Core Focus | Critical Compliance Item |
|---|---|---|
| OT | Surgical safety, infection control | Surgical safety checklist, sterilization records |
| ICU | Critical care quality, HAI prevention | HAI bundles, staffing ratios, documentation |
| Emergency | Triage accuracy, rapid response | Triage system, crash cart readiness, MCI plan |
Common Gaps Found During NABH Assessments
If you are preparing your hospital for NABH accreditation, knowing where hospitals commonly fail can save you a lot of time. Auditors frequently flag issues like:
- Missing or incomplete surgical safety checklists
- Crash cart registers not updated daily
- Lack of documented ICU admission and discharge criteria
- Staff without proper training records or certifications
- No documented mock drill for MCI in the past 12 months
- Sterilization logs incomplete or biological indicator tests not documented
- HAI data not being collected, analyzed, or acted upon
These are fixable issues, but they require a systematic internal audit well before the NABH team walks through your doors. A solid quality assurance and quality control process for hospital projects can help you catch these gaps early and build a culture of continuous compliance.
How to Prepare Your Hospital for NABH Compliance
Getting ready for NABH accreditation in your OT, ICU, and Emergency Department is not a one-time effort. It is an ongoing commitment to quality. Here is a practical approach:
- Gap Analysis: Start with a thorough self-assessment against the NABH standards document. Map out what you have and what you are missing.
- Policy Development: Create written policies for all key areas including triage, sterilization, HAI bundles, and crash cart management.
- Staff Training: All staff in these three departments must be trained on relevant protocols. Keep training records.
- Mock Drills: Conduct drills for MCI, fire emergencies, and cardiac arrest. Document the outcomes and any corrective actions.
- Internal Audits: Set up a regular internal audit system to keep compliance continuous rather than event-driven.
- Quality Indicators: Collect and analyze quality data regularly, such as SSI rates, VAP rates, triage compliance, and crash cart check compliance. It also helps to go through a detailed hospital commissioning checklist to make sure every department is fully ready before operations begin.
Conclusion
NABH standards for OT, ICU, and Emergency Departments are not just bureaucratic checkboxes. They represent a real, evidence-based framework for keeping patients safe and care quality high. For any hospital that wants to build trust with patients, improve clinical outcomes, and stay ahead in a competitive healthcare market, working toward NABH compliance in these critical departments is one of the smartest steps you can take. It requires effort, staff buy-in, and consistent monitoring, but the results — fewer errors, better patient experiences, and a culture of accountability — make it completely worth it.
Frequently Asked Questions (FAQs)
1. What is the difference between NABH entry-level and full accreditation for OT standards?
NABH entry-level accreditation is designed for smaller hospitals and has a simplified set of standards that serve as a stepping stone toward full accreditation. For OT-specific standards, entry-level focuses on basic surgical safety checklists, consent processes, and sterilization practices, while full accreditation requires deeper compliance including advanced infection surveillance, documented quality indicators, and validated sterilization cycles with complete records.
2. How often does NABH audit the ICU for HAI rates?
During the NABH accreditation cycle (which runs for three years), hospitals are expected to continuously collect HAI data (VAP, CAUTI, CLABSI) every month. This data is reviewed both internally and during NABH surveillance assessments, which typically happen once or twice within the accreditation period. Hospitals must show a trend toward improvement or at least a maintained low rate.
3. Is the WHO Surgical Safety Checklist mandatory under NABH?
NABH strongly recommends and practically mandates the use of a surgical safety checklist aligned with the WHO model. While the exact format may vary slightly from hospital to hospital, the three-phase check (Sign In, Time Out, Sign Out) is expected to be in place and documented for every surgical procedure. Non-compliance with this during an assessment is considered a major gap.
4. Can a hospital get NABH accreditation if only its Emergency Department meets the standards?
No. NABH accreditation is a hospital-wide process. The OT, ICU, and Emergency Department are assessed as part of a broader evaluation that includes all clinical and support departments. However, specific NABH programs like the Emergency and Trauma Care Standards do allow focused accreditation for ED services, separate from full hospital accreditation.
5. What are the most common reasons hospitals lose NABH accreditation after getting it?
The most frequent reasons include allowing safety practices to slip after the initial accreditation (like stopping daily crash cart checks or skipping surgical safety checklists), failure to maintain training records for new staff, not updating policies when clinical guidelines change, and inadequate documentation of quality improvement activities. NABH accreditation requires sustained effort, not just a one-time push.